1. WHAT IS DISSOCIATIVE IDENTITY DISORDER ?
Dissociative Identity Disorder (DID) is a mental disorder formerly known as Multiple Personality Disorder (MPD).
The disorder is characterized by the presence of one or more alters (identities) who take it in turns to take control of the person.
The different identities that can be found in DID are called “Alters”.
Alters are not all the same. They may not have the same gender, age or personality. They may also differ in language. One Alter may speak English while all the others speak French, for example. They won’t have the same beliefs, cultures or behavior. Each Alter has its own memories, with some retaining memories of traumatic events while others have none at all.
DID is a disorder that is still controversial in the scientific community. For a long time, it was mixed up with schizophrenia, for example.
Dissociation often stems from traumatic experiences in childhood, when identity is being formed.
Dissociation is a response to traumatic or stressful experiences which may be physically or psychologically threatening. It can also be seen as a coping strategy that helps people avoid the pain and emotional stress associated with traumatic events.
Two forms of DID :
There are two different forms of TDI :
- Possessive form of TDI : This form is represented by alters taking control of the host’s behavior.
- Non-possessive form of TDI :The person remains present, but people verbalize that several alters are manifesting through them.
Prevalence and causes
Given the difficulty of diagnosing DID, its stigmatization and the complexity of the disorder, it can be difficult to estimate prevalence.
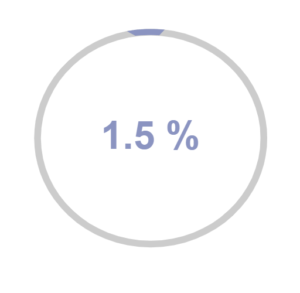
However, according to studies, 1 to 1.5% of people have been reported to suffer from DID.
DID is also more common in people who have suffered repeated childhood trauma, particularly sexual, physical or emotional abuse. Research shows that up to 90% of people with IDD have experienced childhood trauma.
These childhood traumas may have led to problems with emotional regulation and changes in brain development.

2. SYMPTOMS
→ Symptoms of DID include the presence of two or more alters who take control of a person’s behavior on a recurrent basis.
People with DID may also have significant memory gaps for traumatic or stressful events.
Some alters will have a traumatic memory, with the various memories that have weakened their identity, while other alters will have no memory of these events, retaining only the best.
In this way, alters with no traumatic memories are protected from the difficult things they may have experienced.
Other common symptoms of DID can include behavioral and emotional changes, flashbacks, nightmares and hallucinations. People with DID may also have difficulty forming healthy relationships and maintaining a stable self-image.

Dissociative Identity Disorder (DID) is a complex and rare psychological disorder characterized by a fragmentation of identity into several dissociated personality states.
People with DID often experience symptoms that can affect their daily lives and emotional well-being.
Here are some of the most common symptoms of DID :
Dissociative amnesia
People with DID often experience significant memory loss for parts of their lives. These memory losses are caused by dissociated personality states that are responsible for the events that occurred during that period.
Sleep disorders
Sleep disorders, including nightmares and insomnia, due to the anxiety and confusion surrounding their dissociated state.
Self-mutilation and risk behaviors
They may also engage in risky behaviors such as self-harm, eating disorders and risky sexual behavior. These behaviors may be linked to different personality states, beliefs, and needs.
Flashbacks and hallucinations
People with DID may experience flashbacks and hallucinations related to traumatic events that have caused the fragmentation of their identity into different personality states. These flashbacks and hallucinations can be very disturbing and difficult to manage. These symptoms are linked to Post Traumatic Stress Disorder (PTSD).
Personality changes
People with DID often have personality alterations that manifest as changes in behavior, attitude and beliefs. Different personality states may have different names, different ages, different voices and different ways of expressing themselves. For example, a woman in her early 20s may be a 3-year-old male alter.
Depersonalization and derealization
People with IDD may experience feelings of depersonalization and derealization. These reactions are often protective.
In depersonalization, the person feels as if he or she sees him- or herself from outside the body, and experiences all events without being anchored in the body.
While derealization is an altered perception of reality, people may feel that nothing around them is real.
Anxiety and depression
People with IDD can suffer from anxiety and depression due to the confusion and uncertainty surrounding their dissociated personality state.
Different personality states may have different beliefs, emotions and needs, which can make it difficult to understand oneself and communicate with others.
3. DIAGNOSIS
Diagnosing IDD can be difficult due to the complex and variable nature of the symptoms. People with IDD may be misdiagnosed with other disorders such as depression, anxiety, schizophrenia or bipolar disorder. Diagnosis can therefore take a long time.
4. TREATMENT
Psychotherapy :
Psychotherapy seems to be one of the most recommended solutions for dissociative identity disorder.
Common therapeutic approaches for DID include cognitive-behavioral therapy, interpersonal therapy, group therapy and dissociation-focused therapy. Therapy may also include stress management, relaxation and mindfulness techniques.
In psychotherapy, the aim is to try to bring the different personalities together into a single personality. If this is not possible, the aim is to enable the different alters to live together as harmoniously as possible.
- Cognitive-behavioural therapy :
Cognitive-behavioural therapy can help treat symptoms such as depression and anxiety by helping the person to change negative thoughts and behaviours.As we saw earlier, dissociative identity disorder is closely linked to other psychological disorders.
Cognitive-behavioral therapy will help the person to manage the emotions associated with these disorders.
Work on post-traumatic stress can also be undertaken, with the alters holding the traumatic memories. Right from the start of therapy, the person learns to differentiate between the different alters, or at least some of them.
- Group therapy :
Group therapy can be useful for people with IDD, as it can offer emotional and social support. Group therapy can also help improve social skills, foster self-confidence and improve communication with others.
- Hypnosis therapy :
Hypnosis therapy can help explore dissociated memories and strengthen the links between different personality states. Hypnotherapy can be useful in treating symptoms such as anxiety, phobias and flashbacks.
Medication
Medications, such as antidepressants and mood stabilizers, can also be used to treat symptoms associated with DID.
5. PREVENTION
Preventing DID is challenging because risk factors are often beyond the individual’s control. However, efforts to prevent childhood trauma and abuse are crucial to reducing the risk of developing DID.
When trauma occurs, timely and appropriate intervention can help reduce the long-term negative effects on the person’s mental and physical health.
CONCLUSION
Dissociative Identity Disorder is a complex mental disorder characterized by the presence of two or more distinct identities or personalities that recurrently take control of a person’s behavior. People with DID also have significant memory gaps, particularly for traumatic or stressful events. This amnesia is due to the fact that these memories are only present in certain alters.
It is important to note that DID is a rare disorder and most people who experience trauma do not develop it. However, for those diagnosed with DID, psychological therapy can help improve the quality of life and reduce symptoms.
Ultimately, DID remains a controversial topic in the field of psychology and psychiatry due to its unique and complex nature. Nevertheless, mental health professionals continue to explore the underlying causes and treatments to help those affected by this disorder overcome their difficulties and lead fulfilling lives.
